Testosterone deficiency, popularly known as “low T”, has entered the center stage in both the lay and medical communities. However, how is testosterone deficiency (a.k.a. hypogonadism) diagnosed? What is the testosterone level threshold below which you can say you have low T? What are the references ranges for healthy men?
Here you will find out what the medical guidelines say, what critical information they are ignoring, what you should point out to your doctor if he/she doesn’t think you have low T…
What do current clinical practice guidelines say about how to diagnose testosterone deficiency?
The Endocrine Society clinical practice guideline recommends making a diagnosis of testosterone deficiency only in men with consistent symptoms and signs, who also have unequivocally low blood testosterone levels.[1] They recommend testosterone therapy for men with symptomatic androgen deficiency, with the goal to improve their sexual function, sense of well-being, muscle mass and strength, and bone mineral density.
The Endocrine Society clinical practice guideline is against starting testosterone therapy in patients with:[1]
– Prostate cancer or prostate-specific antigen (PSA) greater than 4 ng/ml or greater than 3 ng/ml in men at high risk for prostate cancer (such as African-Americans or men with first-degree relatives with prostate cancer without further urological evaluation).
– Hematocrit greater than 50%.
– Severe lower urinary tract symptoms with International Prostate Symptom Score (IPSS) above 19,
– Uncontrolled heart failure.
When testosterone therapy is instituted, we suggest aiming at achieving testosterone levels during treatment in the mid-normal range with any of the approved formulations, chosen on the basis of the patient’s preference, consideration of pharmacokinetics, treatment burden, and cost. Men receiving testosterone therapy should be monitored.[1]
What are the testosterone reference ranges for men?
The normative reference ranges for total and free testosterone levels in healthy young men vary among assays and laboratories.[2] While variation between laboratories for the same testosterone assay (analytical method) is negligible, it should be noted that reference intervals for testosterone levels (as well as LH and FSH) differ widely and significantly between assays.[3]
In some laboratories, the lower limit of the normal range for total testosterone level in healthy young men is 280–300 ng/dl (9.8–10.4 nmol/liter), and the lower limit of the normal range for free testosterone level (measured by the equilibrium dialysis method) is 5–9 pg/ml (0.17–0.31 nmol/liter).[1]
According to the medical guidelines, clinicians should use the lower limit of the normal range for healthy young men established in the specific assay that is used.[1]
However, it should be noticed that many assays have established testosterone reference ranges that were compiled from small convenience samples of subjects [3-6], and frequently used unreliable laboratory analytics based on the immunoassay technique [7], whose accuracy, particularly in the low range, has been questioned.[2, 8-19] Importantly, the immunoassay technique, which is the most widely used method for measuring total testosterone levels, overestimates true levels and has very limited accuracy at levels below 300 ng/dl.[8] Another study found that over 60% of the samples tested (with testosterone levels within the adult male range) measured by most commercial assays had a spread of up to +/- 20% of those reported by LC-MS (liquid chromatography mass spectrometry) [9], which is the gold standard testosterone analytical method.[19, 20]
Table 1 shows the most recently published reference ranges for total and free testosterone levels, established in a large population of healthy young men aged 19-40 years [21] and older men aged 70-89 years [22], using the gold standard LC-MS analytical method.
TABLE 1. Distribution of total and free testosterone in reference samples of young and older men.[21, 22]
| Total testosterone (ng/dL)men 19-40 years | Free testosterone (pg/mL) men 19-40 years | Total testosterone (ng/dL)men 70-89 years | Free testosterone (pg/mL) men 73-79 years | |
| Mean level | 724 | 142 | 406 | 56 |
| Highest end of normal range | 1322 | 266 | Data not available | Data not available |
| Lowest end of normal range | 292 | 55 | Data not available | Data not available |
| Reference limit for low-T | 348 | 70 | 184 | 30 |
| Reference limit for high-T | 1197 | 230 | 739 | 91 |
Note:
* To convert total testosterone from nanograms per deciliter (ng/dL) to nanomoles per liter (nmol/L), multiply concentrations in ng/dL by 0.0347
* To convert free testosterone from picograms per milliliter (pg/mL) to picomoles per liter (pmol/L), multiply concentrations in pg/mL by 3.47
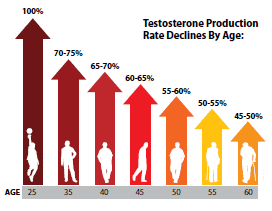
The first thing to note when comparing the reference ranges between young and older men is the dramatic decline testosterone levels. Total testosterone levels in older men are about 40-50% lower than that of younger men. Free testosterone levels drop even more with age. This data confirms findings from previous studies which have shown that as men get older, levels of free (or bio-available) testosterone decline at a faster rate than total testosterone levels.[23-26]
According to the approach used for defining reference limits for biological parameters [27, 28], total and free testosterone values below the 2.5th percentile (approximately 2 SD [standard deviations] below the mean) are deemed low. For total and free testosterone in young men, this corresponds to 348 ng/dL and 70 pg/mL, respectively. The same applies to defining the high end of the reference limit (approximately 2 SD above the mean). For total and free testosterone, this corresponds to 1197 ng/dL and 230 pg/mL, respectively.
As table 1 shows, the normal range for both total and free testosterone is large, going all the way up to 1322 ng/dL in young men. This means that there is a lot of room for expression of different health outcomes when contrasting the low end with the high end of the normal range. In other words, it is very likely that being in the low end will have very different health consequences vs. being in the high end.
I will go into more depth in an upcoming article on what is an optimal testosterone level. As you might have guessed, this is a controversial topic that is generating a lot of heated discussions among both researchers and medical professionals.
Symptoms
As stated by the US Endocrine Society, and also by European medical organizations, the diagnosis of testosterone deficiency requires the presence of symptoms and signs suggestive of testosterone.[1, 29] Table 2 lists symptoms and signs suggestive of androgen deficiency in men, according to the Endocrine Society.
TABLE 2. Symptoms and signs suggestive of androgen deficiency in men.[1]
| More specific symptoms and signs of low-T | Other less specific symptoms and signs of low-T |
| Reduced sexual desire (libido) and activity.Decreased spontaneous erections.Loss of body (axillary and pubic) hair, reduced shaving.Very small or shrinking testes.Inability to father children, low or zero sperm count.Low bone mineral density.Hot flushes, sweats. |
Decreased energy, motivation, initiative, and self-confidence.Feeling sad or blue, depressed mood, dysthymia.Poor concentration and memory.Sleep disturbance, increased sleepiness.Mild anemia (normochromic, normocytic, in the female range). Reduced muscle bulk and strength. Increased body fat. Diminished physical or work performance. |
Questionnaires
Several questionnaires are available to help doctors make a diagnosis of testosterone deficiency according to the current medical clinical guidelines. The Androgen Deficiency in Aging Men (ADAM) and the Aging Male Survey (AMS) questionnaires are two examples.[30, 31] Table 3 shows what you will get asked in the ADAM questionnaire.[31]
Table 3: The Androgen Deficiency in Aging Males (ADAM) questionnaire.[31]
1. Do you have a decrease in libido (sex drive)?
2. Do you have a lack of energy?
3. Do you have a decrease in strength and ⁄ or endurance?
4. Have you lost height?
5. Have you noticed a decreased enjoyment of life?
6. Are you sad and ⁄ or grumpy?
7. Are your erections less strong?
8. Have you noticed a recent deterioration in your ability to play sports?
9. Are you falling asleep after dinner?
10. Has there been a recent deterioration in your work performance?

If the answer is ‘yes’ to question 1 or 7, or at least 3 of the other questions, you might have a low testosterone level.
While the ADAM and AMS questionnaires may be useful rough screening tools to screen for hypogonadism across the adult male lifespan [30], it should be noted that they (like all other questionnaires) are non-specific, i.e. lack diagnostic accuracy.[30] In other words, a man who doesn’t fulfill the criteria can still have low testosterone levels, and vice versa, a man who does fulfill the criteria can have testosterone levels in the normal range. Therefore, the symptoms and signs related to low testosterone levels are only suggestive, not diagnostic of hypogonadism.
Critical problems with the current diagnostic criteria for testosterone deficiency
1. The assumption that there is a specific testosterone level threshold below which the symptoms appear, and that this threshold is the same for everybody.
2. Neglect of the fact the different symptoms often correspond to difference testosterone levels.
3. Ignorance of the fact that testosterone levels in the higher end of the normal range confer health benefits beyond merely symptomatic relief of classical symptoms and signs.
4. Inordinate focus on total testosterone levels, as opposed to free testosterone levels, and not taking into account influence of too low or too high estradiol (the primary estrogen) levels on men’s health.
Next…
Diagnosis and treatment of testosterone deficiency is a controversial topic due to the great inter-individual variability in expression of symptoms and sign related to various testosterone levels, and the lack of clear-cut thresholds at which specific symptoms/signs arise.
In the next article I will start tackling each of the problems with the current diagnostic criteria for testosterone deficiency, and alert you on important issues to bring up at your next doctor visit.
References:
1. Bhasin, S., et al., Testosterone therapy in men with androgen deficiency syndromes: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab, 2010. 95(6): p. 2536-59.
2. Bhasin, S., et al., The impact of assay quality and reference ranges on clinical decision making in the diagnosis of androgen disorders. Steroids, 2008. 73(13): p. 1311-7.
3. Sikaris, K., et al., Reproductive hormone reference intervals for healthy fertile young men: evaluation of automated platform assays. J Clin Endocrinol Metab, 2005. 90(11): p. 5928-36.
4. Eskelinen, S., et al., Biochemical reference intervals for sex hormones with a new AutoDelfia method in aged men. Clin Chem Lab Med, 2007. 45(2): p. 249-53.
5. Tennekoon, K.H. and E.H. Karunanayake, Serum FSH, LH, and testosterone concentrations in presumably fertile men: effect of age. Int J Fertil, 1993. 38(2): p. 108-12.
6. Boyce, M.J., et al., Are published normal ranges of serum testosterone too high? Results of a cross-sectional survey of serum testosterone and luteinizing hormone in healthy men. BJU Int, 2004. 94(6): p. 881-5.
7. Mohr, B.A., et al., Normal, bound and nonbound testosterone levels in normally ageing men: results from the Massachusetts Male Ageing Study. Clin Endocrinol (Oxf), 2005. 62(1): p. 64-73.
8. Rosner, W., et al., Position statement: Utility, limitations, and pitfalls in measuring testosterone: an Endocrine Society position statement. J Clin Endocrinol Metab, 2007. 92(2): p. 405-13.
9. Wang, C., et al., Measurement of total serum testosterone in adult men: comparison of current laboratory methods versus liquid chromatography-tandem mass spectrometry. J Clin Endocrinol Metab, 2004. 89(2): p. 534-43.
10. Taieb, J., et al., Testosterone measured by 10 immunoassays and by isotope-dilution gas chromatography-mass spectrometry in sera from 116 men, women, and children. Clin Chem, 2003. 49(8): p. 1381-95.
11. Kushnir, M.M., et al., Performance characteristics of a novel tandem mass spectrometry assay for serum testosterone. Clin Chem, 2006. 52(1): p. 120-8.
12. Salameh, W.A., et al., Validation of a total testosterone assay using high-turbulence liquid chromatography tandem mass spectrometry: total and free testosterone reference ranges. Steroids, 2010. 75(2): p. 169-75.
13. Demers, L.M., Testosterone and estradiol assays: current and future trends. Steroids, 2008. 73(13): p. 1333-8.
14. Cawood, M.L., et al., Testosterone measurement by isotope-dilution liquid chromatography-tandem mass spectrometry: validation of a method for routine clinical practice. Clin Chem, 2005. 51(8): p. 1472-9.
15. Vicente, F.B., et al., Measurement of serum testosterone using high-performance liquid chromatography/tandem mass spectrometry. Clin Chem Lab Med, 2006. 44(1): p. 70-5.
16. Gallagher, L.M., L.J. Owen, and B.G. Keevil, Simultaneous determination of androstenedione and testosterone in human serum by liquid chromatography-tandem mass spectrometry. Ann Clin Biochem, 2007. 44(Pt 1): p. 48-56.
17. Turpeinen, U., et al., Determination of testosterone in serum by liquid chromatography-tandem mass spectrometry. Scand J Clin Lab Invest, 2008. 68(1): p. 50-7.
18. Thienpont, L.M., et al., State-of-the-art of serum testosterone measurement by isotope dilution-liquid chromatography-tandem mass spectrometry. Clin Chem, 2008. 54(8): p. 1290-7.
19. Soldin, S.J. and O.P. Soldin, Steroid hormone analysis by tandem mass spectrometry. Clin Chem, 2009. 55(6): p. 1061-6.
20. Vogeser, M. and K.G. Parhofer, Liquid chromatography tandem-mass spectrometry (LC-MS/MS)–technique and applications in endocrinology. Exp Clin Endocrinol Diabetes, 2007. 115(9): p. 559-70.
21. Bhasin, S. and S. Basaria, Diagnosis and treatment of hypogonadism in men. Best Pract Res Clin Endocrinol Metab, 2011. 25(2): p. 251-70.
22. Yeap, B.B., et al., Reference ranges and determinants of testosterone, dihydrotestosterone, and estradiol levels measured using liquid chromatography-tandem mass spectrometry in a population-based cohort of older men. J Clin Endocrinol Metab, 2012. 97(11): p. 4030-9.
23. Ferrini, R.L. and E. Barrett-Connor, Sex hormones and age: a cross-sectional study of testosterone and estradiol and their bioavailable fractions in community-dwelling men. Am J Epidemiol, 1998. 147(8): p. 750-4.
24. Muller, M., et al., Endogenous sex hormones in men aged 40-80 years. Eur J Endocrinol, 2003. 149(6): p. 583-9.
25. Litman, H.J., et al., Serum androgen levels in black, Hispanic, and white men. J Clin Endocrinol Metab, 2006. 91(11): p. 4326-34.
26. Feldman, H.A., et al., Age trends in the level of serum testosterone and other hormones in middle-aged men: longitudinal results from the Massachusetts male aging study. J Clin Endocrinol Metab, 2002. 87(2): p. 589-98.
27. Solberg, H.E., International Federation of Clinical Chemistry (IFCC), Scientific Committee, Clinical Section, Expert Panel on Theory of Reference Values, and International Committee for Standardization in Haematology (ICSH), Standing Committee on Reference Values. Approved Recommendation (1986) on the theory of reference values. Part 1. The concept of reference values. J Clin Chem Clin Biochem, 1987. 25(5): p. 337-42.
28. Elveback, L., The population of healthy persons as a source of reference information. Hum Pathol, 1973. 4(1): p. 9-16.
29. Wang, C., et al., Investigation, treatment, and monitoring of late-onset hypogonadism in males: ISA, ISSAM, EAU, EAA, and ASA recommendations. J Androl, 2009. 30(1): p. 1-9.
30. Morley, J.E., et al., Comparison of screening questionnaires for the diagnosis of hypogonadism. Maturitas, 2006. 53(4): p. 424-9.
31. Morley, J.E., et al., Validation of a screening questionnaire for androgen deficiency in aging males. Metabolism, 2000. 49(9): p. 1239-42.





Another great article from Monica. Will factor this in to my next regular blood test and take this info. with me to my doctor. I am not suffering those symptomes, but will be good to see where I am at as I will be about 48 when I do my next blood test. Really looking forward to the follow up article on this on addressing low T. Also, it would be good to have an article about reducing excessive eostrogen in both men and women as this causes big problems for both genders. Thanks.
I’m glad you find the article relevant.
As I will explain in the upcoming follow-up article, having non-symptomatic low T should be addressed as well because higher levels (in the reference range) confer health benefits regardless presence/absence of symptoms.
I will cover the issue of estrogen as well. Stay tuned! 🙂
Great job, Monica. Dr. Joseph Mercola had a recent article about Low-T and expressed concern about the development of cancer, if a man undergoes Low-T therapy. Both you and Will Brink say the opposite. It’s rather confusing, if you know what I mean. I’d be happy to send you Mercola’s article, if you want to read it. Let me know. Thanks.
Yes, please post the link here and I will be happy to take a look at it. Thanks.
As mentioned in the past, Mercola is not a reliable source of health information.
Thanks, Will, as always, for your input. While some of his articles are good, in my opinion, others are questionable. He seems to back up his claims with evidence, but that can’t always be relied upon.
Happy Thanksgiving to you, sir!
Ditto Kent!
Great job Monica!
You provided some information here that I have been attempting to locate. Very interested in reviewing the population used for the reference group in establishing the “normal” range for Testosterone in young healthy men.
I’m going to differ with you on one point though. Serum free testosterone has low diagnostic value because it fluctuates significantly, is unstable in serum and has an upper reference range limit that is very low compared to that of young healthy men.
Androstanediol Glucuronide, the first metabolite of DHT, has the highest diagnostic value (because it’s an indicator of how much testosterone has acted). Next is total testosterone combined with SHBG and lastly free testosterone.
They were healthy men 19-40 years. You can look it up in the study:
Yeap, B.B., et al., Reference ranges and determinants of testosterone, dihydrotestosterone, and estradiol levels measured using liquid chromatography-tandem mass spectrometry in a population-based cohort of older men. J Clin Endocrinol Metab, 2012. 97(11): p. 4030-9.
I clinical practice, serum free testosterone is not measured directly, it is calculated using SHBP and albumin as variables. Total testosterone has a circadian rhythm, and therefore so will the free fraction.
The MS analytic method can detect low T (as well as estradiol) levels seen in hypogonadal men and women.
While androgen glucuronide profiling holds promise as an indicator of androgenic activity, eg:
Labrie F, Be´langer A, Be´langer P, Be´rube´ R, Martel C, Cusan L,
Gomez J, Candas B, Castiel I, Chaussade V, Deloche C & Leclaire J.
Androgen glucuronides, instead of testosterone, as the new
markers of androgenic activity in women. Journal of Steroid
Biochemistry and Molecular Biology 2006 99 182–188.
…this lab technique is still confined to research labs and not available yet in clinical practice.
When you say “highest diagnostic value” you have to be more specific. As I will outline in the upcoming article, some androgen dependent effects have been found to be more strongly correlated with free T levels than total T levels.
Thanks for the reply.
I agree with you that total T is overemphasized in practice, however free T is not very useful unless you are referring to 24 hour urine. Yes, free and total T fluctuate with the circadian rhythm, free T varies far more than total outside of the typical 24 hour cycle. Historically, endocrinologists have only treated rarer, severe deficiencies rather than mild or borderline deficiencies that are very common and contribute to decreased quality of life and the degenerative diseases. As you know lab data is always interpreted with respect to a patient’s history, complaints and physical signs. Free T just isn’t as useful in clinical practice for this because of it’s inherent variability (free T may be fine for severe deficiencies).
Total T – more stable than Free T
Androstanediol Glucuronide (AG) – provides direct evidence of metabolic impact of DHT.
Enriched with SHBG and Estradiol
AG is commercially available at one or more of the major national labs (of course most docs have not heard of it, much less be capable of correlating it to a medical complaint). I had it ordered lat year at Lab Corp in 2012.
I know you are very well informed and this doesn’t apply to you. Most reachers are no more informed in a particular subject than the physicians that apply their findings. This is what leads to all the ridiculous, sloppy science we see like fish oil causes prostate disease.
To make matters worse, the hard sciences have determined that consensus (a political concept) is somehow relevant to the scientific method. If you look at the Endocrine Society’s Clinical Practice Guidelines, each starts out declaring that it’s a consensus document. They form a committee, debate the issue and vote. If there is consensus fine, if not there can be compromise. Utterly asinine.
The endocrine society’s symptoms for deficiency is woefully incomplete. This leads to reachers taking these symptoms that were formed out of a consensus process and testing them for validity. Some may be correct, however they end up leaving others out.
What do you mean by “Enriched with SHBG and Estradiol”?
As I will outline in upcoming articles, there are many issues with the Endocrine Society’s Clinical Practice Guidelines.
You say “free T is not very useful”. While it is harder to accurately measure than TT (total T), one can still monitor whether levels increase or decrease in response to interventions. If measured under the same circumstances, the direction of change itself can give clues. Some studies have identifies that free T correlate stronger with certain outcomes than TT, eg:
Free testosterone levels are associated with mobility limitation and physical performance in community-dwelling men: the Framingham Offspring Study.
Krasnoff JB, Basaria S, Pencina MJ, Jasuja GK, Vasan RS, Ulloor J, Zhang A, Coviello A, Kelly-Hayes M, D’Agostino RB, Wolf PA, Bhasin S, Murabito JM.
J Clin Endocrinol Metab. 2010 Jun;95(6):2790-9
AG is a relatively new analytic method; while it holds promise, at this time there is no data upon which one can develop a quantitative relationship between metabolites of testosterone (or DHEA or other androgens) and the dose requirements for individual patients. But science is constantly evolving, so we might hear more about the measurement of androgen metabolites and their possible clinical use, in the future. Another interesting emerging technique is the use of metabolomics (ie comprehensive measurement of the total low-molecular weight or metabolite content of a cell, tissue or body fluid) for the improved diagnosis, therapy and monitoring of T deficiency.
All I meant by enriched was those 2 additional tests add information to the clinical picture.
In terms of Free T, it’s not the test method that I have a problem with, it’s that free T isn’t stable. It fluctuates widely in blood. So, we end up with a wide reference range that make it more difficult to interpret. Even more problematic is that the optimal free T level in men is higher than the typical reference range (typically 250-350 pg/mL). Healthy young adults often >300 pg/mL.
If you haven’t done so, please see:
The Hormone Handbook, 2nd edition
Thierry Hertoghe, MD
He backs up all of this and much more with 400 pages of just references, categorized by hormone and specific problem. He includes, for example, cutoff blood levels for specific symptoms and the reference to support the position.
Please take a look at this reference before you publish the next article. There is so much information here that most physicians have never heard. It is referenced and backed up by research.
I’m looking forward to seeing what you do next.
Total testosterone concentrations are measured by RIA, immunometric assays, or liquid chromatography tandem mass spectrometry. Automated assays for total testosterone are available in most hospital laboratories and usually are sufficiently accurate to distinguish eugonadal from hypogonadal men ( 18 , 19 ). Total testosterone levels are affected by alterations in SHBG that occur in obesity, old age, diabetes mellitus, hyper- and hypothyroidism, and acromegaly, and in men taking certain medications (Table 2 ⇑ ). Accurate and reliable assays for free or bioavailable testosterone measurements usually are not available in local laboratories, and these tests should be performed in a reliable reference laboratory. Free testosterone measurements by analog methods are frequently available in local laboratories, but these measurements are affected by alterations in SHBG and are inaccurate ( 19 ). Their use is not recommended. Free testosterone level can be measured accurately by equilibrium dialysis or calculated from total testosterone, SHBG, and albumin ( 20 ). The calculated free testosterone concentrations are dependent on the quality of total testosterone and SHBG assays. The calculated free testosterone concentrations differ systematically from those measured by equilibrium dialysis and vary with the algorithm used for calculating free testosterone ( 21 ). Bioavailable testosterone is measured by ammonium sulfate precipitation or calculated from total testosterone and SHBG.
Monica, you are amazing. I appreciate your in-depth research along with the clear and definitive method you use to present your research. I very much enjoy your papers and your great . . . well . . . let’s say the results of your dedicated exercise. Rock on.
I’m glad you appreciate the results of my brain exercise as well as physical exercise, thank you. 🙂
Great Articles Monica 😀 Well done. Can you please tell me, is my free T ok ? Because, my total T is in the lower range and my SHBG is low also ? Is this good or no. I am feeling great, my libido was always skyhigh and I have pronounced hairiness since early puberty. Will be better for me to increase total T ? I am 24 years old, and down there is my bloodwork from two years ago
LH 11,5 + mIU/mL (1.7 – 8.6)
FSH 3.7 mIU/mL (1.5 – 12.4)
Progesterone 0.47 ng/mL (0.20 – 1.40)
Prolactin 317 uIU/ml (86 – 324)
Testosterone 3.46 ng/mL (2.80 – 8.00)
Estradiol 22.84 pg/mL (7.63 – 42.60)
Cortizol 818 nmol/L 8-10 (175-536)
16-20 (64-327)
SHBG 12.0 – nmol/L (14.5 – 48.4)
DHEA-S 339 μg/dL (————-)
TSH 3.280 uIU (0.270 – 4.200)
T3 1.8 nmol/L (1.3 – 3.1)
T4 108 nmol/L (66-181)
Before I say anything I want to make it clear that I am not a doctor. With that being said, I can comment on your labs and give you my opinion.
My fist question is; what time did you do the blood draw?
You are only 24, so you total T level should be much higher, ideally in the 8-12 ng/ml range (or 900-1200 ng/dl).
Because your total T level is so low, even though your SHBG is low (which is inversely correlated with free T), your absolute free T level will be low also.
Your DHEA-S is low end also. Its reference range for a man you age is 280 – 640 ug/dL:
http://www.nlm.nih.gov/medlineplus/ency/article/003717.htm
Your LH is high, which means that your body is trying to elevate your testosterone production. I suggest you get the same blood test again (including DHT) in about 5-6 months. If your total T level is still low, then TRT might be appropriate for you. Go to an endocrinologist who specialize in androgen issues.
You didn’t provide your blood lipid, lipoprotein or CRP (C-reactive protein, an inflammatory marker) numbers. If those are out of range, then that would be another indication for you to get on TRT.
You say you don’t have any symptoms; that’s good, but pay attention to this as you get older.
You are amazing. Thank you. I appreciate your quick and detail answer.
This is my last bloodwork few moths ago at 9 AM (alo hormonal panel was taken at 9 AM)
Lipid profile:
Total cholesterol: 5.8 (0,00- 5,70) mmol/L H
Triglycredides: 1,47 (0,00 – 1,71)mmol/L
HDL 1,07 (0,90 – 3,10)mmol/L
LDL 4,01 (0,00 – 4,12)mmol/L (I know that my HDL-LDL ratio is not ideal 🙁 )
Also my blood panel:
WBC 5.11 (4.000-9.60)
RBC 5.49 (4.37-5.63)
HgB 166 (135.00-165.00)
HcT 46.3 (40.00-50.00)
MCV 84.20 (82.00-100.00)
MCH 30.30 (26.20-33.60)
MCHC 360 (316-337)
RDW 13.90 (10-15)
PLT 254 (144-400)
MPV 6.9 (6.50-11)
Glucose 5.0 (4.20 – 6.40)
SE 2 (0.00-10.00)
PT (protrombin time) 12.2 (10-14)
I do not have CRP ? (I do not know what is it, will search for it today 🙂 )
I will also check all of this you recommended in you previous replay before going to endocrinologist and have a nice talk with him 🙂 Do I need something else to check and talk about with endo ? Thank you very much again 🙂
You’re welcome. 🙂
Good you did your blood draw in the morning. T levels are highest in the morning and display a circadian rhythm, so it is important to measure at around the same time in order to get reliable data.
A large body of research have shown that TRT has beneficial effects in middle-age and older men. There is less data on this in young men. So this is something you and your doctor will have to find out.
Thank you, will do 🙂 Waiting for new articles :p
Hey Marko,
Your thyroid may be low as well. If we were treating your lab form like most physicians today will do, then your levels are mildly deficient at a minimum.
Best practice is to interpret the lab data with respect to your physical symptoms and complaints.
Correcting thyroid function can increase the efficiency and production of other hormones.
Hi, Jim, I have done blood analasys again few days ago, but thyroid hormones are optimal.
These findings showed worse condition than bloodwork two years ago from my previous post.
This is TRT condition i think 🙁 Will probably start with 125 mg test enanthate every week. Do I need HCG in TRT for fertility reasons ? I will soon go to endo and talk about enanthate prescription.
Morning blood 8:30 AM>>>
LH 4.6 mIU/mL ( 1.7 – 8.6 )
Testo 2.27- ng/mL (2.80 – 8.00 )
FSH 3.0 mIU/mL ( 1.5 – 12.4 )
SHBG 15.1 nmol/L (14.5 – 48.4 )
Prolactin 406+ uIU/mL ( 86 – 324 )
11:00 AM Prolactin 347+ uIU/mL ( 86 – 324 )
1:00 PM Prolactin 271 uIU/mL ( 86 – 324 )
8:30AM Cortisol 722+ nmol/L (175 – 536 ) ACTH: 32 pg/mL ( 7 – 63 )
4:00PM Cortisol 356+ nmol/L (64 – 327 ) ACTH: 21 pg/mL ( 7 – 63 )
TSH 2.300 uIU/mL (0.270 – 4.200 )
FT4 20 pmol/L (12 – 22 )
blood 11 AM: >>>
LH 9.0+ mIU/mL ( 1.7 – 8.6 )
Testo 1.54– ng/mL (2.80 – 8.00 )
FSH 3.0 mIU/mL ( 1.5 – 12.4 )
SHBG 14.0 nmol/L (14.5 – 48.4 )
Blood 1 PM: >>>>
LH 7.3 mIU/mL ( 1.7 – 8.6 )
Testo 1.70-ng/mL (2.80 – 8.00 )
FSH 3.0 mIU/mL ( 1.5 – 12.4 )
SHBG 13.8 nmol/L (14.5 – 48.4 )
Forgot to mention E2 7.49 (7.6 – 42.6) pg/ml
Something is sideways with your prolactin. It could be inhibiting testosterone production. The etiology of the elevated levels should be determined.
FSH and estradiol levels are responsible for spermatogenesis. Your e2 level is low. Adding testosterone will likely increase E2 and SHBG.
You and your doc will watch FSH and E2. If they become elevated you can either lower E2 with an aromatase inhibitor or add HCG. Adding small amounts of testosterone should not inhibit testosterone production as long as E2 levels are properly managed.
Run down the elevated prolactin.