Will has previously mentioned DHEA as it relates to hormonal effects and health promotion:
http://www.brinkzone.com/general-health/dhea-hormone-facts
http://www.brinkzone.com/articles/dhea-the-most-underrated-supplement-for-women
http://www.brinkzone.com/articles/xv-international-symposium-on-atherosclerosis
When it comes to health promotion and longevity, DHEA is a supplement which deserves more attention than it is getting.
DHEA levels (the main circulating form of DHEA in the bloodstream is DHEAS) decrease approximately 80% between ages 25 and 75 year.[1, 2] This large decline in DHEA has led to interest in the possibility that aging related DHEA deficiency may play a role in the deterioration in physiological and metabolic functions with aging, and in the development of chronic diseases.
In support of this, it has been reported that DHEA level is negatively correlated with mortality and risk of developing cardiovascular disease (CVD) (i.e. lower DHEA(S) levels are associated with higher mortality and CVD risk).[3-5] More recently it has been found that a steep decline or extreme variability over time in DHEA(S) levels is associated with higher mortality, more so than baseline DHEA(S) levels.[6]
Aging not only reduces DHEA(S) levels, but also results in an increase in arterial stiffness [7, 8], which is an independent predictor of cardiovascular disease (CVD) risk and mortality.[9-11] It has been reported that DHEA levels are inversely associated with arterial stiffness (i.e. lower DHEA levels are associated with increased arterial stiffness. [7, 12, 13] Therefore, it is possible that DHEA replacement could reduce arterial stiffness, and thereby contribute to reduction in CVD and mortality…
Objective
A notable study sought to determine whether DHEA replacement therapy in older adults reduces indices of arterial stiffness; carotid augmentation index (AI) and carotid–femoral pulse wave velocity (PWV).[14]
Methods
A randomized, double-blind trial was conducted to study the effects of supplementing with 50 mg DHEA per day on AI and PWV in women and men aged 65–75 year. Inflammatory cytokines and sex hormones were also measured in fasting serum.
Results
For both men and women, compared to placebo, DHEA supplementation increased total testosterone, free testosterone index, estradiol, and free estradiol index, as outlined in the table (values are means):
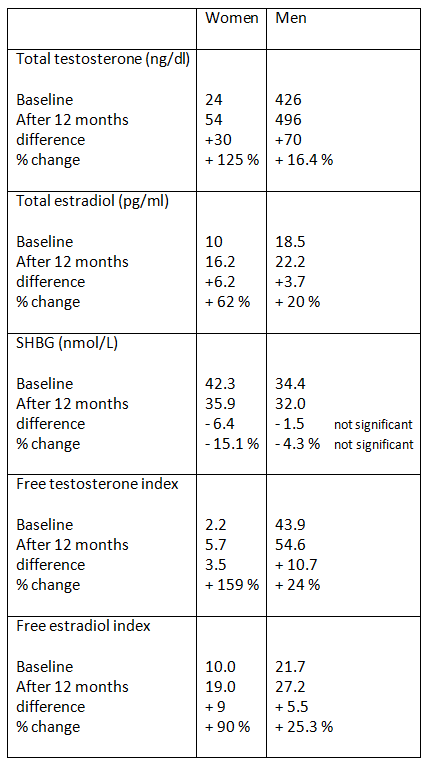
Notes:
Free testosterone index and free estradiol index is the ratio of total testosterone or estradiol to SHGB.
The free testosterone index was calculated as (total testosterone x 0.0347)/SHBG, where testosterone is expressed in ng/dL and SHBG in nmol/L.
The free estradiol index was calculated as (total estradiol x 0.00367)/SHBG, where estradiol is expressed in pg/mL and SHBG in nmol/L.
AI significantly decreased by 24% in the DHEA groups (no difference between men and women), but not in the placebo groups.
Pulse wave velocity also decreased; however, after adjusting for baseline values, the between-group comparison became non-significant.
The reductions in AI and PWV were accompanied by decreases in inflammatory cytokines (TNF-alpha and IL-6) and correlated with increases in serum DHEAS. The reductions in AI also correlated with free testosterone index. There were no differences between men and women, with respect to the DHEA-induced changes in inflammatory markers.
In the supplemented groups, DHEA supplementation also decreased plasma triglycerides (blood fats) by 11.6 % (14 mg/dl), and there were tendencies for reductions in BMI and body weight with DHEA supplementation.
There were no serious adverse events attributable to DHEA replacement in either men or women.
This study confirms that DHEA supplementation for 1 year is safe. Supplementing with DHEA 50 mg/day for 1 year does not significantly alter lipid profile or adversely affect the endometrium in postmenopausal women.[15] And earlier study showed that supplementing with 50 mg DHEA per day for 2years is safe for both men and women.[16]
This study also confirms the improvement in plasma triglycerides and inflammatory cytokines (IL-6 and TNFα) seen in a previous study, which further demonstrated that DHEA supplementation 50 mg/day for 1 year decreases insulin resistance and improves glucose tolerance in elderly men and women.[16] An earlier study also showed improvement in insulin sensitivity, and in addition, a 10% reduction in intra-abdominal fat mass (i.e. visceral fat, measured by MRI) in both men and women.[17]
DHEA replacement in elderly men and women improves indices of arterial stiffness (reduces AI and PWV) and enhances arterial elasticity. The 24% decrease in AI that was observed with DHEA supplementation is large in the context of arterial aging. Based on a 0.30 percentage point per year increase in AI during adulthood [8], the DHEA-induced reduction in AI is equivalent in magnitude to a 20-year reversal of arterial aging.
Furthermore, based on a meta-analysis that shows that every ten percentage point increase in AI corresponds with a approximately 36% greater risk for cardiovascular and all-cause mortality during a 4-year follow-up period [18], the reductions in AI that we observed would be expected to correspond with a 17% reduction in mortality risk.[19] Therefore, the improvements observed in this study suggest that DHEA replacement might partly reverse arterial aging and reduce the risk for cardiovascular and the metabolic syndrome.
The hormonal data in this study (see the table) confirms the less known fact the postmenopausal women have lower estradiol levels than men of the same age. It further shows that DHEA has a greater beneficial impact in women on the ratio of free testosterone (index) to free estradiol (index) than in men. In men, it increases free testosterone (index) and free estradiol (index) roughly equally.
The beneficial outcomes of this and related long-term studies substantiates the safety and health promoting effects of DHEA supplementation, and give you another reason to go and get your blood level of DHEA(S) checked. Strive to keep it in the upper end of the normal reference range. If your level is low, regardless of adrenal insufficiency (a disorder of deficient cortisol production), a good starting dose is 50 mg per day. As the studies outlined in this article show, this is a safe and effective long-term dose for both men and women. Check your blood levels of DHEA(S), testosterone, estradiol and SHBG (as well as glucose and insulin) after about 6 months supplementation. Ideally you want to check these before you start supplementing with DHEA as well in order to establish your baseline so you can see the impact of the supplementation.
While most research showing health promoting effects of DHEA have been done in older men and women, the need for DHEA supplementation should be dictated by your blood DHEA(S) level. Thus, even if you are younger, if your level is low, supplementing with DHEA as a primary prevention approach will most likely benefit you in the long run as you get older.
References:
1. Orentreich, N., et al., Age changes and sex differences in serum dehydroepiandrosterone sulfate concentrations throughout adulthood. J Clin Endocrinol Metab, 1984. 59(3): p. 551-5.
2. Orentreich, N., et al., Long-term longitudinal measurements of plasma dehydroepiandrosterone sulfate in normal men. J Clin Endocrinol Metab, 1992. 75(4): p. 1002-4.
3. Barrett-Connor, E., K.T. Khaw, and S.S. Yen, A prospective study of dehydroepiandrosterone sulfate, mortality, and cardiovascular disease. N Engl J Med, 1986. 315(24): p. 1519-24.
4. Berr, C., et al., Relationships of dehydroepiandrosterone sulfate in the elderly with functional, psychological, and mental status, and short-term mortality: a French community-based study. Proc Natl Acad Sci U S A, 1996. 93(23): p. 13410-5.
5. Mazat, L., et al., Prospective measurements of dehydroepiandrosterone sulfate in a cohort of elderly subjects: relationship to gender, subjective health, smoking habits, and 10-year mortality. Proc Natl Acad Sci U S A, 2001. 98(14): p. 8145-50.
6. Cappola, A.R., et al., Trajectories of dehydroepiandrosterone sulfate predict mortality in older adults: the cardiovascular health study. J Gerontol A Biol Sci Med Sci, 2009. 64(12): p. 1268-74.
7. Hougaku, H., et al., Relationship between androgenic hormones and arterial stiffness, based on longitudinal hormone measurements. Am J Physiol Endocrinol Metab, 2006. 290(2): p. E234-42.
8. Vaitkevicius, P.V., et al., Effects of age and aerobic capacity on arterial stiffness in healthy adults. Circulation, 1993. 88(4 Pt 1): p. 1456-62.
9. Laurent, S., et al., Aortic stiffness is an independent predictor of all-cause and cardiovascular mortality in hypertensive patients. Hypertension, 2001. 37(5): p. 1236-41.
10. Cohn, J.N., Arterial stiffness, vascular disease, and risk of cardiovascular events. Circulation, 2006. 113(5): p. 601-3.
11. Sutton-Tyrrell, K., et al., Elevated aortic pulse wave velocity, a marker of arterial stiffness, predicts cardiovascular events in well-functioning older adults. Circulation, 2005. 111(25): p. 3384-90.
12. Dockery, F., et al., The relationship between androgens and arterial stiffness in older men. J Am Geriatr Soc, 2003. 51(11): p. 1627-32.
13. Fukui, M., et al., Relationship between low serum endogenous androgen concentrations and arterial stiffness in men with type 2 diabetes mellitus. Metabolism, 2007. 56(9): p. 1167-73.
14. Weiss, E.P., et al., Dehydroepiandrosterone replacement therapy in older adults improves indices of arterial stiffness. Aging Cell, 2012. 11(5): p. 876-84.
15. Panjari, M., et al., The safety of 52 weeks of oral DHEA therapy for postmenopausal women. Maturitas, 2009. 63(3): p. 240-5.
16. Weiss, E.P., et al., Dehydroepiandrosterone (DHEA) replacement decreases insulin resistance and lowers inflammatory cytokines in aging humans. Aging (Albany NY), 2011. 3(5): p. 533-42.
17. Villareal, D.T. and J.O. Holloszy, Effect of DHEA on abdominal fat and insulin action in elderly women and men: a randomized controlled trial. JAMA, 2004. 292(18): p. 2243-8.
18. Vlachopoulos, C., et al., Prediction of cardiovascular events and all-cause mortality with central haemodynamics: a systematic review and meta-analysis. Eur Heart J, 2010. 31(15): p. 1865-71.
19. Vlachopoulos, C., K. Aznaouridis, and C. Stefanadis, Prediction of cardiovascular events and all-cause mortality with arterial stiffness: a systematic review and meta-analysis. J Am Coll Cardiol, 2010. 55(13): p. 1318-27.







Intersting article, being in my 50’s it’s always good to know what supplements or hormones are good. there are to many things that just don’t work but promise the earth. DHEA not only increases Testosterone which is good for us older guys but helps with CVD as well a double whamy which is even better. Getting hold of it is the problem for me in the UK. If you don’t have a sympathetic doctor who will prescribe it then it’s over the internet but who would you trust to buy it from that’s the question. I will have to some research on this. Monica we need more on DHEA there is not lot on the net about it (well not on trusted sites at least).
Although DHEA appears to have a number of potential benefits, it’s a poor choice for increasing testosterone in men. It appears to give a boost in T levels for women (see linked article above) it’s a poor choice for men for that specific effect mostly due to the increase in estradiol. At the doses used for general healthy, such as covered above, it’s a non issue.
Good point Will. Men shouldn’t expect any hormonal benefit from DHEA (except those who have extremely low estrogen levels). Take DHEA for its health benefits; get your level to mid/high range and have your level stay there.
Thanks for another well written article Monica.
One additional point is that senescence is associated with deficiency in almost all the major hormones. Testosterone, DHEA, aldosterone, vasopressin, cortisol, thyroid, gh/IGF-1, thyroid, oxytocin, pregnenalone etc.
DHEA also has a critical role in cortisol supplementation. About 1/3 of aging adults have a cortisol deficiency. When supplementing it’s important to include DHEA plus T to neutralize the catabolic effects of cortisol.
well written and well documented article .. I have no real medical background so these articles are very helpful/… I’ve been taking 25mg a day DHEA for a couple of years… definitely increases agro… in me anyway.. I don’t take any other sups other that the standard protein creatine glutamine and BCAA’s and multivitamins… …
Interesting. I have heard that DHEA is a benefit to improved aging. I have high HDL and low tiglycerides.
I will try a diet of 50mg peer day. However, wondering if I increased it to 100 or 150mg per day is beneficial. I read one study where women took 200mg of DHEA with no side effects. Any comment? Health risks going over 50mg/da.?
Start with 50 mg/day and get you blood test; no point to increase the dose if your DHEA(S) level is already high. I’d say 100-150mg/day is a safe dose. But again, let your blood level dictate how much to take.
Any Brink approved brands for which to buy DHEA?
Or would using the same companies that we get our other supps from
be sufficient.
Get your DHEA from a large reputable brand like Life Extension or Vitacost, and you’ll be fine.
Thanks, Monica